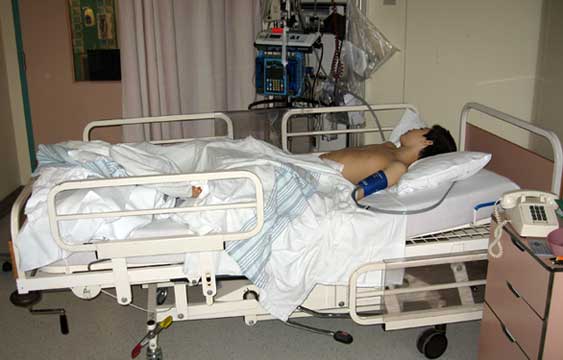
 So today can be summed up with the image/feeling of me with my head on Jon’s chest, trying to sooth him, as he alternated between groaning in pain and trying to sit up and tear at his zimmers/epidural/catheter.
So today can be summed up with the image/feeling of me with my head on Jon’s chest, trying to sooth him, as he alternated between groaning in pain and trying to sit up and tear at his zimmers/epidural/catheter.
In hindsight, we can reconstruct what happened. The epidural started leaking on Thursday—maybe even Wednesday night post-surgery—but they were able to compensate by increasing the dosage and Jon had a good night last night.
But it was likely the wear-and-tear of shifting him from bed to table for the x-rays this morning that did it. By the time we got Jon up to his bed, he couldn’t get comfortable and you could see another site where the anaesthetic was leaking in a little river from the fine tube taped down along his spine. Then a tech came into examine his zimmers and she stroked his feet. Up until then Jon could feel a tap, but he showed no foot reflexes. When the tech brushed them, I saw Jon’s toes arch out. Uh oh, it looked like he was gaining fully sensation in his legs. And within an hour all he was suffering.
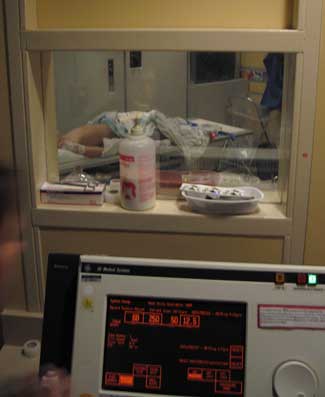
View from the X-ray Control Room
Our nurse Patti quickly started the protocol to get morphine going and remove the epidural. Powerful medications, so it takes time. So it was about two hours before Jon started getting comfortable again, but it wasn’t true comfort. The epidural removes sensation, the morphine just dulls the pain.
Jon has been pretty dopey the rest of the day. Despite the pain stress on Jon, nurse Patti insisted on getting Jon out of bed and into a wheelchair this afternoon. This is to get his body back into a more natural position ASAP, to aid in healing.
Last year, we were very impressed with how the hospital handles pain, especially compared to five years previously. Every morning you are visited by a triumvirate from the Pain Management Team, who assess and decide the course of the treatment for the next 24 hours and beyond. Of course, now we know that last time was the ideal situation — the epidural lasted well, and Jon’s pain transition was ideal. But epidurals are not predictable, and this time we got to see how they react when things are not ideal…and I’m equally impressed.
Because Jon can’t give a great introspective analysis of his pain, we can only read his body and manner and fly by the seat of our pants. In cases like ours, we are brought into the decision huddle and our opinions are given a goodly amount of weight. (From right out of surgery, we were brought in to consult on how Jon was reacting to pain.) So the pain situation may not be ideal, but we are a respected part of the process searching for a solution, and that makes all the difference.
Still, here at home, late on my off-night, my thoughts return to lying my head on his chest, trying to absorb some of Jon’s pain.

 This what we’ll be dealing with for the next 12 weeks or more. What you’re looking at is a big white styrofoam wedge, with velcro straps wrapping around two grey zimmers (the overgrown shinguards also known as “knee immobilizers”).
This what we’ll be dealing with for the next 12 weeks or more. What you’re looking at is a big white styrofoam wedge, with velcro straps wrapping around two grey zimmers (the overgrown shinguards also known as “knee immobilizers”). 
 We’re definitely getting down to the short strokes now: Jon’s been completely de-tubed, with the IV coming out around dinnertime. Nice, substantial dinner; then at around 7 p.m. we’ve had our first poop (which apparently—from Jon’s expressions—was akin to giving birth). We’re waiting for a visit from the physiotherapist—about the only reason they want us to hang around until tomorrow.
We’re definitely getting down to the short strokes now: Jon’s been completely de-tubed, with the IV coming out around dinnertime. Nice, substantial dinner; then at around 7 p.m. we’ve had our first poop (which apparently—from Jon’s expressions—was akin to giving birth). We’re waiting for a visit from the physiotherapist—about the only reason they want us to hang around until tomorrow.

